If you’ve spent years being told your legs are just heavy, that you need to move more, or that it’s simply water retention — you’re not alone. So many women who come to us have been on a long and exhausting road before they finally get answers.
Lipoedema is a chronic condition involving abnormal fat accumulation — most commonly in the legs, and sometimes the arms. It causes real, physical symptoms: pain, swelling, easy bruising, and over time, increasing difficulty with mobility. And critically, it doesn’t respond to diet or exercise the way typical fat does.
Understanding what a lipoedema assessment actually involves — what doctors look for, how the condition is staged, and what comes next — can make the process feel a lot less daunting. So here’s what to expect.
What is a Lipoedema Assessment?
A lipoedema assessment is a medical evaluation to determine whether your symptoms are consistent with the condition. It typically focuses on three things: identifying the clinical signs of lipoedema, confirming or ruling out a diagnosis, and understanding how far the condition has progressed.
Unlike many conditions, lipoedema can’t be confirmed through a blood test. Diagnosis is clinical, meaning it’s based on your history, what a doctor observes, and sometimes imaging. This is why seeing a doctor who actually understands lipoedema matters so much.
A thorough assessment may also help identify related conditions affecting the veins or lymphatic system, which can influence how your care is managed.
Why Getting a Proper Diagnosis Matters
Lipoedema is misdiagnosed constantly. Women are regularly told their symptoms are caused by obesity, hormonal weight gain, fluid retention, or lymphoedema — and they leave appointments without real answers, often feeling dismissed.
But lipoedema fat behaves differently from typical fat tissue. It doesn’t shift with diet changes. It doesn’t respond to exercise. And it comes with pain, tenderness, and bruising that can significantly affect quality of life. Without a proper diagnosis, those symptoms just keep being explained away.
A proper lipoedema assessment gives you clarity. It lets you finally put a name to what you’ve been experiencing — and opens the door to a management plan that’s actually designed for your condition.

Signs Lipoedema Doctors look for During an Assessment
Recognising the clinical signs of lipoedema is central to the diagnostic process. Here’s what doctors are typically looking for.
Symmetrical Fat Distribution
One of the most distinctive features of lipoedema is that both sides of the body are affected equally. Both legs will be enlarged, and the fat distribution tends to stop abruptly at the ankles or wrists — leaving the feet and hands largely unaffected. This can create what’s sometimes described as a “cuff” appearance at the ankle.
Pain and Tenderness in the Affected Tissue
Pain is one of the key features that separates lipoedema from typical fat distribution. Patients often describe pain when pressure is applied, sensitivity to touch, and a persistent feeling of heaviness in the limbs. If you’ve ever wondered why your legs ache in ways that seem disproportionate to your activity level — this could be why.
Easy and Unexplained Bruising
Many women with lipoedema bruise easily — often without a clear cause. Bruises can appear without any obvious trauma, and they may take longer than usual to heal. This happens because the small blood vessels within the affected tissue are more fragile than normal.
Swelling That Worsens Throughout the Day
Some patients notice their legs feel worse after long periods of standing, sitting, or physical activity — and improve again after rest. In earlier stages of lipoedema, this swelling typically spares the feet, which is one of the features that helps distinguish it from lymphoedema.
How Lipoedema is Diagnosed
A lipoedema diagnosis usually brings together a few different elements.
Your Medical History
Your doctor will want to understand when your symptoms first appeared, whether anyone in your family has experienced similar issues, and whether there’s a link to hormonal changes like puberty, pregnancy, or menopause. These life stages are commonly associated with the onset or progression of lipoedema, so this context matters.
Physical Examination
A hands-on examination will look at fat distribution patterns, skin texture, areas of nodularity within the tissue, and where swelling is occurring. This helps determine whether your symptoms fit the criteria for a lipoedema diagnosis and, if so, at which stage.
Ultrasound or Vascular Imaging
Some clinics incorporate imaging as part of their assessment. Ultrasound can help evaluate the health of the veins, check for secondary lymphoedema, and rule out other vascular causes of swelling. At Lipoedema Surgical Solution, Dr Lekich and his team use ultrasound-guided diagnosis to get a full picture of your leg health — including any underlying conditions that could affect your treatment or surgical outcomes.
Understanding Lipoedema Staging
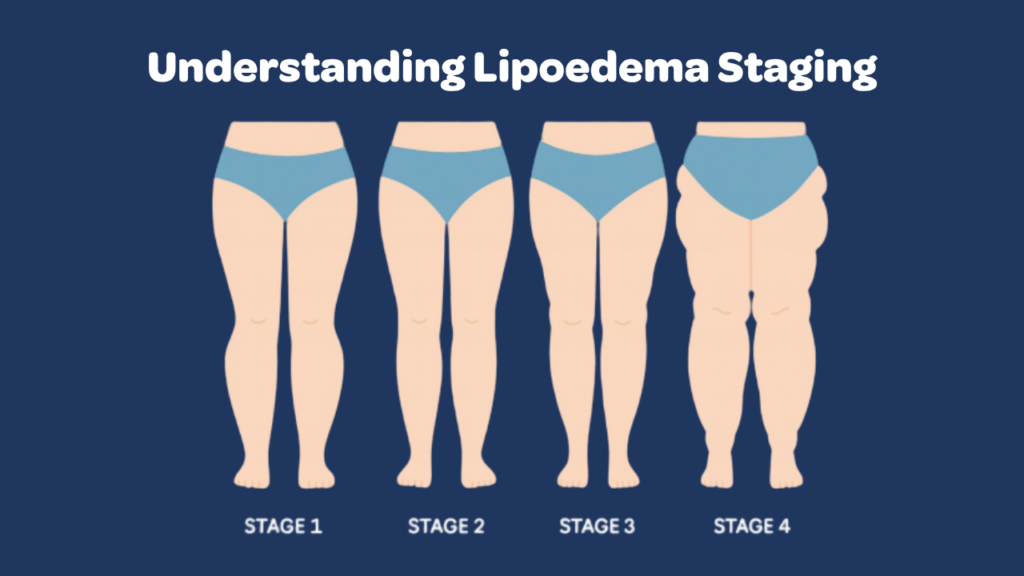
Once a diagnosis is made, doctors will classify the condition using a staging system that describes how far the disease has progressed.
Stage 1
The skin surface is smooth, the tissue underneath is relatively soft, and enlargement of the affected areas is mild. Many women are surprised to learn their Lipoedema was at Stage 1 — it can still cause significant discomfort even at this stage.
Stage 2
The skin may begin to look uneven or dimpled. Fat tissue becomes thicker and nodules within the tissue become more noticeable.
Stage 3
Larger fat deposits are present, limb shape changes significantly, and skin folds may develop. Mobility challenges become more pronounced at this stage.
Stage 4 — Lipo-Lymphoedema
In advanced cases, secondary lymphoedema can develop alongside Lipoedema. This stage involves persistent swelling, impaired lymphatic drainage, and the swelling may now extend to the feet.
What Happens After a Lipoedema Diagnosis?
A diagnosis isn’t the end of the road — it’s actually where things start to move forward. Following a lipoedema diagnosis, doctors will typically discuss conservative management before considering any surgical options.
This usually includes:
- Flat knit compression garments
- Manual Lymphatic Drainage (MLD)
- Anti-inflammatory dietary changes
These approaches support lymphatic health and help manage symptoms. For patients who have already worked through conservative management and are looking for longer-term relief, surgical options may then be explored.
How the Assessment Process Works at Lipoedema Surgical Solution
We know that walking into a clinic for the first time can feel overwhelming, especially after years of being misunderstood by the medical system. That’s why our process is designed to educate and support you before any in-person testing.
It starts with a group information session hosted by Dr Chris Lekich, where he explains lipoedema, walks through possible treatment pathways, and answers questions. From there, you’ll have a one-on-one telehealth consultation to discuss your individual symptoms and history in more detail.
Following your telehealth consultation, you’ll receive a diagnosis and a personalised conservative management plan. All of this can happen from home — so you can start getting clarity and taking steps forward without needing to travel for an initial appointment.
When to Seek a Lipoedema Assessment
If any of the following sound familiar, it’s worth reaching out:
- Symmetrical enlargement of the legs or arms that doesn’t respond to diet or exercise
- Pain or tenderness in the affected tissue
- Frequent bruising that appears without obvious cause
- Swelling that gets worse throughout the day or doesn’t shift with typical weight management
A lipoedema assessment can help confirm whether your symptoms align with the condition and, if they do, give you a clear path forward. The earlier you seek answers, the sooner you can begin managing the condition in a way that actually works for your body.
You deserve to feel understood. And you deserve answers.