If you live with lipoedema, you may have noticed that your body reacts in ways that feel hard to explain. Tenderness that doesn’t match what you can see. Sensitivity that flares for no obvious reason. Digestive discomfort. Skin that itches without warning.
These experiences are real, and you are not alone in having them.
In recent years, there has been growing interest in the connection between mast cells, histamine, and the way lipoedema is experienced. This page explores what the research currently suggests and what remains uncertain.
What Is Mast Cell Activation Syndrome?
Mast Cell Activation Syndrome (MCAS) is an immunological condition in which mast cells — a type of white blood cell involved in allergic and immune responses — release chemical mediators more readily or in greater quantities than usual. Histamine is one of the most well-known of these mediators, but mast cells can release hundreds of different signalling chemicals.
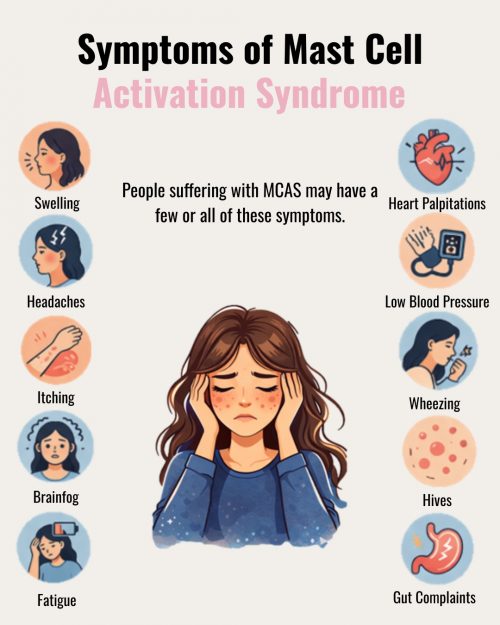
Symptoms associated with MCAS can vary considerably between individuals and may include flushing or redness of the skin, itching or heightened skin sensitivity, digestive symptoms such as bloating or discomfort, headaches or migraines, fatigue and cognitive fog, and nasal congestion or sinus-related symptoms. Because mast cells are present throughout the body – in the skin, gut lining, connective tissue, and around blood vessels – their effects can feel widespread and difficult to attribute to a single cause.
What Do Mast Cells Actually Do?
Mast cells function as first responders within the immune system. They are positioned at key interface points between the body and its environment — along the gut lining, beneath the skin, and adjacent to blood vessels — where they can rapidly detect and respond to perceived threats.
When activated, mast cells release a range of chemical mediators that influence inflammation, blood flow, and tissue sensitivity. This is a normal and important function. In conditions like MCAS, however, this activation may occur more readily, or produce responses that are disproportionate to the trigger.
What is Histamine and Why Does It Matter?
Histamine is a naturally occurring chemical that plays a role in immune responses, digestion, and cell-to-cell communication throughout the body. Among its functions, histamine contributes to the dilation of blood vessels, the regulation of inflammatory signals, and the support of digestive processes.
When histamine activity increases — whether due to higher production, slower breakdown, or both — it can contribute to symptoms such as redness, swelling, itching, and heightened sensitivity. In the context of lipoedema, this has prompted researchers and clinicians to ask whether histamine may influence how symptoms are experienced in some individuals.
Why Is Mast Cell Activity Being Explored in Lipoedema?
The relationship between mast cells, histamine, and lipoedema is an area of active inquiry. It does not yet have definitive answers, but several observations have made it a meaningful subject of discussion.
One notable finding is that mast cells are often concentrated around blood vessels — and changes in vascular structure have been observed in lipoedema-affected tissue. This has led researchers to consider whether altered blood vessel architecture might trigger or amplify mast cell responses in affected areas.
Several theories are currently being explored:
Area of Interest | What Researchers Are Considering |
Mast cell sensitivity | Whether mast cells in lipoedema tissue may be more readily activated |
Mast cell density | Whether more mast cells are present in affected areas than in unaffected tissue |
Immune system involvement | Whether multiple immune cell types — not mast cells alone — contribute to the picture |
Vascular changes | Whether altered blood vessel structure triggers mast cell responses in affected tissue |
Is Lipoedema an Inflammatory Condition?
This is a question that remains open in the research community. Some findings suggest that certain inflammatory pathways may be more active in lipoedema-affected tissue, while others appear normal or reduced. Conventional blood markers used to measure inflammation may not fully capture what is happening at the tissue level.
Inflammation in lipoedema may not follow the patterns typically seen in other conditions — which is part of what makes it a complex and often misunderstood condition.
Rather than focusing on mast cells in isolation, some researchers are considering lipoedema within the context of a broader immune system pattern — one that may involve mast cells, macrophages, T-cells, B-cells, and other inflammatory signalling pathways working in combination.
The Gut, Mast Cells, and Systemic Inflammation
Another area of emerging interest is the connection between gut health and broader inflammatory activity. Mast cells are highly active in the gut lining, and when triggered, they can contribute to changes in intestinal permeability — sometimes described as increased gut permeability.
When this occurs, substances that would normally remain within the gut may enter the bloodstream, prompting a systemic immune response. This process may help explain why some individuals with lipoedema report symptoms that extend well beyond the areas of visible tissue change — including digestive discomfort, fatigue, and sensitivities that seem disproportionate or hard to connect.
Symptoms That May Overlap
Some women with lipoedema describe a pattern of symptoms that may align with mast cell activity. These can include skin tenderness or heightened sensitivity in affected areas, itching, flushing or redness, digestive discomfort, and increased sensitivity to medications, foods, or environmental triggers.
It is important to note that the presence of these symptoms does not confirm mast cell activation, and their absence does not rule out any particular process. These patterns are being explored because they appear in self-reported experience — not because they have been definitively linked to a single underlying mechanism.
Does Mast Cell Activation Cause Lipoedema?
There is currently no evidence to support the idea that mast cell activation syndrome causes lipoedema. The two conditions can co-exist, and mast cell activity may influence how inflammation, sensitivity, and swelling are experienced in some individuals — but they are distinct conditions with distinct presentations.
Understanding this distinction matters, because it shapes how assessment and management are approached. A blanket assumption that mast cell activity is driving lipoedema symptoms may lead to interventions that miss other important factors.
Why This is Gaining Attention
Increased awareness of lipoedema as a recognised condition, a growing body of patient-reported symptom patterns, and emerging research into connective tissue, vascular structure, and immune behaviour have all contributed to greater clinical interest in this area. Researchers and clinicians are increasingly willing to engage with the complexity of lipoedema rather than viewing it through a single lens.
At the same time, it is important to approach emerging theories with measured curiosity. Research in this area is still developing, and no single explanation currently applies to all individuals with lipoedema. The complexity of this condition is part of why personalised, doctor-led assessment matters.
A Broader Picture
Mast cell activation and histamine are one thread in a much larger picture. Lipoedema is likely shaped by multiple interacting systems — fat tissue behaviour, vascular structure, lymphatic function, hormonal influences, and immune signalling among them. Understanding this complexity can help explain why symptom experiences vary so significantly between individuals, and why a one-size-fits-all approach rarely serves people well.
Your symptoms are valid, even when they are hard to explain. Understanding what may be contributing to them is the first step toward finding a path that works for you.
If you’re interested in hearing directly from clinical research, there is a recent podcast discussion where an endocrinologist explores mast cell activation, inflammation, and how this may relate to lipoedema.
What to Do If You Recognise These Symptoms
If you are experiencing persistent swelling, tenderness, sensitivity, or symptoms that feel difficult to explain, a structured medical assessment can help provide clarity. A doctor-led approach considers your full clinical picture — including the many systems that may be involved — rather than focusing on a single pathway or theory.
At Lipoedema Surgical Solutions, our education sessions are designed to give you clear, evidence-informed information in a supportive environment. They are a starting point for understanding your body — not a commitment to any particular path.
Attend a Lipoedema Education Session to learn more about lipoedema and how it may relate to you.